The Shadow Epidemic: Why Long-Term Benzodiazepines Cause More Harm than Good
by Shawn Barnes, M.D.
WHAT IF I OFFERED YOU A PILL?
What if I offered you a pill that lowered your risk of Alzheimer’s disease, hip fractures, car accidents, and lung infections? What if this same pill was likely to improve the quality and restfulness of your sleep, increase your daytime energy level, and improve your mood and cognition? No such magical pill exists; however, each of the benefits listed above can be facilitated by getting off benzodiazepines. You may wonder why I am writing about benzodiazepines for readers who do not prescribe or manage medications, i.e., psychologists, social workers, and marriage and family therapists. Psychotherapists, given the frequency with which they see patients, are often in a position to most clearly see how benzodiazepines are affecting a patient’s cognitive or emotional functioning. They may also play a vital role in supporting any patient who makes the decision to get off their benzodiazepine under the close guidance of their physician.
INTRODUCTION
The most commonly used benzodiazepine medications are Xanax, Klonopin, Ativan, Valium, and Restoril. Most patients I encounter have not gone out seeking benzodiazepines, nor are taking them illicitly. In the most likely scenario, the patient was having a difficult month and saw her psychiatrist or primary care doctor, who prescribed Xanax for sleep or anxiety. Five years later, she is still taking Xanax regularly, and is now suffering from cognitive problems, low energy, low mood, or worsening sleep. To my query about what her doctor told her about the risks of Xanax, she says “Only that it can be addictive.” It falls on me now, to have the difficult discussion about the many risks of long-term benzodiazepines, the likelihood that the benzodiazepines are worsening her symptoms, and the complicated process of coming off them.
HISTORY
Before benzodiazepines, we used medications such as Thalidomide, barbiturates, and opium for sleep or anxiety. When benzodiazepines were introduced in the 1960s, they were heralded as a safe and effective alternative, quickly becoming the most prescribed class of medications in the U.S. in the 1970s (Lopez-Munoz et al., 2011). We may look back and roll our eyes at some of the silly and anachronistic indications for benzodiazepines in the 1970s (See Figure 1, for example). However, I would argue that this type of irresponsible advertising set the stage for why benzodiazepines continue to be casually prescribed today for the “treatment” of normal, nonpathological experiences of the human condition. Unfortunately, benzodiazepines have very real, pathological risks.

Figure 1: Valium Ad from the 1970s
THE SHADOW EPIDEMIC
The problems of addiction and overdose from benzodiazepines are well known. The next time you read about a celebrity opioid overdose death, look for a toxicology report. Odds are that he or she was on a benzodiazepine, as in the case of Michael Jackson, Heath Ledger, Prince, Whitney Houston, Tom Petty, etc. Last year, there were over 10,000 overdose deaths involving benzodiazepines (National Institute on Drug Abuse, 2018), yet doctors continue to prescribe them with ever more frequency. Since the mid-1990s, benzodiazepine overdose deaths have increased by about 400%. During that same time, doctors have written 67% more benzodiazepine prescriptions and the strength (in milligrams) of those prescriptions has risen 300% (Bachuber et al., 2016. See Figure 2). The Opioid Epidemic is rightly getting a lot of press and policy attention, but benzodiazepine use is the shadow epidemic. Addiction and overdose are widely acknowledged risks of benzodiazepines, but there are lesser-known, and potentially more serious problems with these medications.
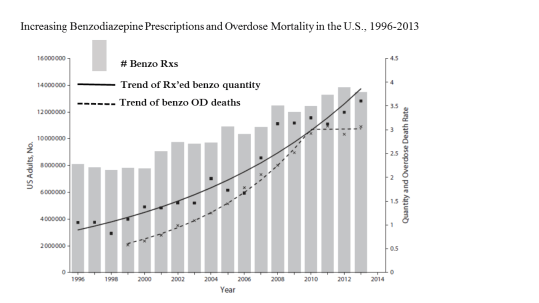
Figure 2 (Modified from Kaufmann et al., 2018)
DEMENTIA
In my clinical experience, some benzodiazepine risks resonate with patients more than others. Patients tend to be less concerned with the prospect of addiction/overdose, because it feels remote and more likely to happen to “someone else.” It’s a shame that addiction/overdose is usually the only risk that doctors discuss with patients, as it tends to give the impression that benzodiazepines are safe, as long as you don’t abuse them. However, in the past decade, mounting evidence indicates that benzodiazepines may increase the risk of Alzheimer’s dementia by 30-80%, depending on dose and length of time exposed (Islam et al., 2016). As we will discuss below, benzodiazepines decrease time in deep-stage sleep. Beta amyloid (the substance that accumulates in neurons and leads to Alzheimer’s) is thought to be cleared from neurons during deep stage sleep (Buscemi et al., 2007). Therefore, one proposed mechanism for the benzodiazepine-Alzheimer’s connection is the accumulation of beta amyloid in neurons by inhibition of deep stage sleep. Of the many risks of benzodiazepines, I find the association with Alzheimer’s disease resonates most with patients. Unfortunately, this risk is seldom mentioned when the prescription is initially offered.
WORSENING SLEEP
Benzodiazepines are powerful sedatives, but tend to worsen overall sleep quality over time. EEG studies have demonstrated that benzodiazepines decrease deep-stage/slow-wave sleep, decrease delta count, increase REM sleep latency, and increase stage 2 non-REM sleep (Poyares et al., 2004), thus resulting in less restful, less restorative sleep. The effect of alcohol on sleep is a good analogy; alcohol works on the GABA neuroreceptor (as do benzodiazepines). GABA modulation (by alcohol or benzodiazepines) can be sedating, but not necessarily followed by a restful, optimal quality sleep. The longer a patient is on benzodiazepines, the more the sleep architecture is disturbed; this is supported by research findings that after patients taper off benzodiazepine, both their subjective and objective sleep quality tend to actually improve (Ashton, 2005)
WORSENING ANXIETY
Clinical data seem to indicate that many people who have been taking benzodiazepines for a long time experience an overall increase of anxiety (Guina & Merrill, 2018). Benzodiazepine users can develop a tolerance for the drug, i.e., they need more medication to get the same anti-anxiety effect after only 4-8 weeks (Bateson, 2002). In addition, benzodiazepines are known to inhibit fear extinction, which is crucial for overcoming anxiety in the long-term. In this way, they can actually hinder recovery from trauma/PTSD and are contraindicated in this condition despite what may be perceived as beneficial effects in the short-term. As with sleep, most people report less anxiety once they have been successfully tapered off long-term benzodiazepines (Ashton, 2005).
OTHER RISKS
In addition to the risks discussed above, long-term benzodiazepines can produce low mood, low daytime energy level, and reduced cognition, often collectively known as “brain fog” (Guina & Merrill, 2018). They are also correlated with higher risks of being in a car accident (Elvik, 2013), falls resulting in hip fractures (Donnelly, et al., 2017), and respiratory infections (Obiora, et al 2013), especially in the elderly.
APPROPRIATE BENZODIAZEPINE USE
As elaborated above, there are many dangers in the long-term use of benzodiazepines, but I would be remiss if I did not mention their benefits when used correctly. Benzodiazepines have an important place in medicine, but their uses are nearly always short-term or intermittent, i.e., not every day, nor for prolonged periods of time. For example, they can be quite helpful for short-term relief from symptoms of alcohol withdrawal, jetlag, specific phobias, or acute anxiety/insomnia. Professional guidelines on prescribing benzodiazepines are clear that they should be used short-term, usually for less than four weeks (Baldwin et al., 2014; Bandelow et al., 2012; Locke et al., 2015; Matheson & Hainer, 2017; Qaseem et al., 2016). However, how many patients have you seen that have been on benzodiazepines for four weeks or less? My guess is not many. Despite these guidelines and the evidence for their long-term adverse effects, 85% of benzodiazepines in the U.S. are prescribed for more than 6 months (Kaufmann et al., 2018). I consider this a public health crisis that, like the opioid epidemic, is primarily the responsibility of physicians. Unfortunately, the American Psychiatric Association has yet to issue guidelines on long-term benzopdiazepine use.
MEDICALLY SUPERVISED BENZODIAZEPINE WITHDRAWAL
We all have patients who have said something akin to, “Wait doc, I know I need to be on Xanax because I once ran out and was off for a few days. My anxiety and insomnia were through the roof! I can’t live life like that. I need my Xanax!” Here the patient is confusing benzodiazepine withdrawal with return of illness, assuming that what they felt during acute withdrawal will be their new baseline. Coming off long-term benzodiazepines can be a profoundly uncomfortable, and medically dangerous, experience. Withdrawal symptoms include intense rebound anxiety/insomnia, hallucinations, depression, heart palpitations, shooting pains, sensitivity to noise and light, suicidal ideation, and seizures (Poyares et al., 2004). The longer a patient is on the medication and the higher the dose, the worse the withdrawal tends to be. Withdrawal from benzodiazepines (unlike other substances) can last for weeks to months, but does wane over time. There are many ways to ease withdrawal, including other medications, herbals, and supplements. Here, I want to emphasize the importance of medical supervision when coming off benzodiazepines. There have been reports of death due to stopping benzodiazepines cold turkey and only a qualified physician, after meeting with a patient and discussing the risks, benefits, and alternatives, should make the decision about whether and how to start the weaning process.
WHAT CAN YOU DO?
As a psychologist or allied mental health professional who conducts psychotherapy, you may understand your patients better than any other health care professional they are seeing. Your patients may trust you and feel more comfortable with you than they do any other health care professional. This provides a safe and supportive space to begin a conversation about what their medication means to them and how they invest themselves in their medication. If a patient has been taking benzodiazepines for years, it would be worthwhile to talk about why they were originally put on it and why they continue to take it. Has their doctor had a full discussion with them about the risks, benefits, and alternatives? Does their doctor keep renewing the prescription without a long-term plan? In my experience, once informed of the risks, benefits, and alternatives, most patients actually want to come off benzodiazepines. Perhaps you can encourage your patient to have an open and honest conversation with their doctor about these issues.
Patients can become physiologically and psychologically dependent on their benzodiazepines, and the topic of re-evaluating their medications should be introduced with skill and sensitivity. As mentioned above, withdrawal from benzodiazepines can be traumatic and a long-drawn-out process; it is vital that they are educated about what to expect and how you can prepare them and support them throughout the process. Your role as a therapist can be invaluable in both encouraging patients to have an honest conversation with their doctor about benzodiazepines, and in facilitating their adjustment to the significant and sometimes scary changes they will experience during and after the withdrawal process. It can be empowering for a patient to achieve a desired and hard-won outcome, and to know that they are able to cope on their own, using their own skills and resources.

Dr. Barnes is an integrative psychiatrist, and has a small, solo practice in Encinitas, Ca. He practices at the intersection of conventional psychiatry, alternative/holistic medicine, and therapy-based approaches. He enjoys having the time to collaborate with therapists and other providers.
Print a copy of this article here.
Thank you for alerting professionals to this very serious issue. I’d like to also add, having worked with thousands of people coming off of benzos, that some people have radical and extreme problems coming off even after 2 weeks use. While that may not be the norm it’s not completely unusual in a population of people having trouble coming off which is largely what I’ve worked with now for a long time. In worst-case scenarios people develop disabling illness for some years. This is something that is often not even recognized or validated by professionals which is extremely traumatizing to people who are going through such issues. People are often told that their withdrawal issues are psychiatric rather than physiological. Again this is devastating given we know that people are truly physiologically hurting, their nervous systems in chaos. Thank you once again. It should be noted that ssris also implicated with many thousands of people having similar horrible withdrawal issues. And in fact neuroleptics and mood stabilizers to cause this sometimes. It’s not as common for thousands of people to come off of mood stabilizers and neuroleptics but it looks like they’re just as problematic. The medical establishment largely denies all of this. This must end. Informed consent needs to be made in every instance of psychiatric drug prescriptions.
LikeLike