Category: 2017
Managing PTSD Symptoms Through Food (or No Food): Trauma, PTSD, and Eating Disorders
by Julie Trim, Ph.D.
Individuals with an eating disorder (ED) who report a history of trauma, or indeed, meet full criteria for post-traumatic stress disorder (PTSD), pose several challenges to the practitioner wishing to deliver evidence-based treatment. ED practitioners may have expertise in eating disorders, but few have strong training or experience with PTSD and associated comorbidities. Working with this subgroup requires specialized training in PTSD assessment and treatment. Diagnosing PTSD can be difficult in ED individuals because ED symptoms can “mask” or suppress PTSD symptoms, and PTSD symptoms can overlap with other psychiatric disorders such as major depressive disorder.

Image credit: http://trauma.blog.yorku.ca/2015/04/look-at-me/
When an ED patient has PTSD, there are certain areas of sensitivity or conflict that arise in ED treatment and present additional barriers to success. The experience of a traumatic event can cause significant shifts in survivors’ views of the world, self, and others. Disruptions in one’s sense of safety, trust, power/control, intimacy, and self-esteem have been shown to be particularly salient in trauma survivors. Anecdotally, it is often these areas that pose additional challenges to treatment for the patient and the clinician alike. For example:
- Safety: In order to preserve a sense of safety, a person who experienced trauma may tell themselves that the trauma occurred due their body size or weight, and that being at a higher or lower weight will keep them safe from future traumas. (“If I hadn’t looked a certain way, I wouldn’t have been raped.”). In fact, these types of self-blaming beliefs maintain or perpetuate PTSD.
- Trust: It is generally difficult for ED individuals to trust their treatment providers with regard to food, weight, and exercise recommendations. With an ED–PTSD patient, there are often additional barriers to trust given that interpersonal traumas (e.g., abuse or assault) often lead to a general distrust of others.
- Power/control: ED–PTSD patients often report feeling “in control” if they are able to make choices about their food and weight, and treatment typically involves letting go and allowing others (e.g., a dietitian) to influence these decisions. For ED–PTSD patients, this seems to trigger a strong pull to regain control and may lead these patients to “dig their heels in” and refuse to follow their team’s recommendations. Power/control issues may also emerge in intensive ED treatment settings, which are highly structured and supervised. The rules of the treatment center may lead ED–PTSD patients to feel extremely safe (i.e., one of the only safe places they have) or could be perceived as an unnecessary restriction of their rights, power, and control.
All of these sensitivities (i.e., safety, trust, and power/control) make sense given the patient’s history. However, they can lead to a “bumpy road” in treatment and, in some cases, may result in dropout or premature termination from treatment.
ED-PTSD individuals can present with a range of diagnoses and behaviors. With respect to ED behaviors, binging and purging are typically more prominent than food restriction in this subpopulation. Researchers have speculated that overeating or binging becomes a self-soothing strategy for a traumatized individual, as these behaviors decrease emotional arousal and “numb” or suppress unpleasant feelings and memories. Purging serves a similar function, and can occur as a way to counteract an episode of binge eating. Outside of their ED diagnosis, ED patients with PTSD individuals tend to have significantly more comorbidities than those without PTSD; these include substance use disorders, mood disorders, impulse control disorders, and borderline personality disorder (BPD).
Formulating a treatment plan for a patient with an ED and PTSD is not easy, to say the least. ED practitioners are faced with complex questions: When to start PTSD treatment? What type of PTSD treatment to use? When to pause or stop PTSD treatment (if a problem arises)? Although research on the types of trauma experienced by individuals with EDs, comorbidity rates, and so forth is abundant, clear guidelines for treating ED-PTSD patients are lacking. ED clinicians are generally aware that trauma-related symptoms often represent a major obstacle to ED recovery, and yet clinicians are often fearful that starting PTSD treatment will trigger increased ED behaviors as well as other worrisome behaviors like self-harm, substance abuse, and suicidality. In a recent study by Kathryn Trottier, Ph.D. and colleagues, ED clinicians cited several barriers to providing PTSD treatment to their patients, including: (1) uncertainty about how to integrate trauma work with ED treatment, (2) lack of training in trauma-focused treatment, (3) institutional financial constraints, (4) not an institutional priority, (5) belief that trauma-focused treatment is a “long-term” endeavor, (6) preference for individualized treatment, (7) perceived readiness of the patient for trauma-focused work, and (8) concerns about psychiatric decompensation. Approximately half of participating clinicians anticipated at least four of these barriers, and 12% anticipated all eight.
Decisions about the treatment plan are fairly arbitrary given the limited research in this area. Possibly the least arbitrary—although still complex—is determining when the patient is ready for PTSD treatment. In some cases, other problems should be addressed prior to starting PTSD treatment (e.g., danger to self/others, safety concerns, and psychological conditions that interfere with the patient’s ability to receive or benefit from PTSD treatment), but PTSD treatment can be started as soon as these issues are resolved (Resick et al., 2014). Tim Brewerton, M.D., a prolific researcher in this area, argued that PTSD treatment should not begin until (1) the patient indicates a readiness to begin trauma work, (2) the patient is adequately nourished and able to process information emotionally and cognitively, (3) the patient’s eating disorder symptoms are relatively under control, and (4) the patient has demonstrated an adequate level of distress tolerance.
Due to its clear structure in addressing multiple behaviors and treatment targets, Dialectical Behavior Therapy (DBT; Linehan, 1993) lends itself well to treatment with these patients. The DBT hierarchy monitors patient safety, minimizes behaviors that undermine or interfere with therapy, and provides a framework or “road map” for treatment. Melanie Harned, Ph.D., has developed a protocol for integrating Prolonged Exposure (PE; one of the four evidence-based treatments for PTSD) with DBT. The DBT PE protocol may not only enhance treatment effectiveness but also allow ED practitioners to feel less trepidatious delivering PTSD treatment to their patients. Furthermore, because many PTSD patients would like to be free of PTSD symptoms, making PTSD treatment contingent on elimination of higher treatment targets (i.e., life-threatening behavior and therapy-interfering behavior) can be a highly effective strategy for both reducing the severity of PTSD and meeting higher treatment targets.
To our knowledge, the Eating Disorders Center at UC San Diego is the only program in the country that provides evidence-based PTSD treatment for ED patients in a partial hospitalization program (PHP) or intensive outpatient program (IOP). In our Adult Program, patients can choose between Prolonged Exposure (PE) and another evidence-based PTSD treatment, Cognitive Processing Therapy (CPT). Post-treatment follow-up of patients who have participated in UC San Diego’s ED+PTSD program have shown positive outcomes.
Print a copy of this article here.

Dr. Trim is an Assistant Clinical Professor and Director of Adult Services at the UC San Diego Eating Disorders Center. She serves as co-chair of the Trauma Special Interest Group (SIG) at the Academy for Eating Disorders and speaks internationally about the treatment of trauma and eating disorders.
“No soy DACA, ni soy de allá”
I am not from Here nor There
by Mariela Shibley, Ph.D.
The title is play of words based on a song written by the late Argentinian composer Facundo Cabral, “No soy de aquí, ni soy de allá.”
When I was 13 years old, my parents decided to leave my country of birth, Argentina, and drag me along with them to the United States. With the passing of time, I learned English and slowly adapted to the American culture, but I always held on to my Argentine roots. Not being able to adjust my immigration status for years, I lived in the shadows – paying thousands of dollars in non-resident tuition so I could attend community college and altering my social security card so that I could get a job. Most of my friends did not know that I was undocumented because of the shame and fear I felt. When I was finally able to return to Argentina years later, I was treated like a visitor. It was then when the title of one of Facundo Cabral’s songs began to play over in my head: “No soy de acá, ni soy de allá,” which translates to “I am not from here, nor there.” This dichotomy has been the core of my experience as an immigrant, and how many immigrants feel as well.

Art installation depicting Immigration at the U.S.-Mexico Border in Tecate, Baja California by French artist, JR
The United States has become home for many individuals who were brought to the country as young children with their families. Many were brought when they were infants and have never gone back to their native country, making the United States the only country they have ever known and the place they call home. These children grow up speaking English as their first – and sometimes only – language, and since they are undocumented and thus unable to travel internationally, they have never left the United States. Many of these children do not find out about their immigration status until they graduate high school, when they attempt to obtain a driver’s license or to enroll in college. Imagine the shock, the confusion, and the frustration these young people feel. They did not choose to come to this country and be uprooted from their native land. And they certainly did not decide to be subjected to all the obstacles they face as a result of being undocumented. Suddenly, these young people realize that they and their families are different from other American families. Due to the negative stigma associated with being undocumented, these young kids tend to keep their undocumented status a secret from their peers. They suffer in silence, feeling alienated from their American friends and sometimes distanced or resentful toward their parents, who brought them here in the first place.
Efforts to fix this problem date back to August of 2001, when congress failed to pass a bipartisan act called the DREAM Act (Development, Relief, and Education for Alien Minors), a bill that would provide conditional permanent residency to certain young immigrants who meet specific requirements. In June of 2012, President Barack Obama signed an executive order to curb the deportation of certain young undocumented immigrants. This policy, known as the Deferred Action for Childhood Arrivals (DACA), allows certain undocumented immigrants who entered the United States as minors to obtain a renewable work permit and may prevent their deportation. They are able to apply for a driver’s license, join the military, and in some U.S. states they can attend universities and qualify for in-state tuition. DACA was a compromise for the DREAM Act. Although it is not in and of itself a path to citizenship, it allows these undocumented individuals to build a future for themselves and to contribute to society. Almost 800,000 Dreamers* between the ages of 16 and 36 are currently able to attend college and graduate school, to work, and to pay taxes because of this program. They do not have to live in fear of being deported for not having legal immigration status. Their U.S. citizen relatives do not have to fear being separated from those they love most and their families being torn apart.

Art Installation, “Eyes of a Dreamer,” spanning both countries across the U.S.-Mexico Border in Tecate, Baja California by French artist, JR
This past September 5, the new administration announced that it will rescind the DACA program. For those currently in the program, their permits to work and attend college will begin expiring in March of 2018 – unless Congress passes legislation allowing a new channel for temporary or permanent legal immigration status. Trapped in a broken immigration system, intelligent and hard-working youth must confront an uncertain future because of the barriers to continuing their education, working, or joining the military. These 800,000 young people, who once felt a sense of hope and who have been contributing to this country’s growth, are now faced with having to go back to the shadows. They fear being deported from the country they call home – the only country they know – to a foreign land. As President Obama (2017) said in a beautiful Facebook post: “These Dreamers are Americans in their hearts, in their minds, in every single way but one: on paper.”
Immigrating to a new country entails numerous losses: the loss of one’s familiar surroundings, their loved ones, possibly language, and even culinary customs, amongst others. The extent to which a person is able to accept such losses determines one’s ability to adapt to the new host culture (Volcan, 1993). For example, a person who was forced to leave their familiar surroundings and who does not want to rescind their customs and way of life will have a much harder time adapting to the new environment and culture, especially if it is very different from what they are accustomed to. This is also mitigated by age (older individuals tend to struggle more than young children) and whether the relocation will open doors to a more prosperous future.
Individuals whose departure is involuntary are more prone to experience culture shock – a general feeling of disorientation due to a sudden introduction to an unfamiliar culture, environment, and way of life (Garza-Guerrero, 1974). This unleashes a stressful, anxiety-laden process whereby one struggles to adapt to the changes while grieving the losses inherent in the transition. The combination of mourning such profound personal losses and a forceful introduction to a new environment challenges the stability of a person’s psyche (Akhtar, 1995).
One can only imagine the negative effects that being removed from the United States, the only country many of these young Dreamers know, will have on them. It’s true, these people who were brought to this country are not from here, but they are also not from there. Regardless of what Congress decides to do about these 800,000 Dreamers, damage has been done by highlighting the fact that they do not belong. And believe me, it hurts.
Note: *Dreamers are those who would qualify for benefits under the DREAM Act, even though such act has not been made into law. They are immigrants who were brought to the United States as children (prior to age 16), who have been residing in this country continuously since 2007, and who were younger than 31 years of age by June of 2012.
References
Akhtar, S. (1995). A third individuation: Immigration, identity, and the psychoanalytic process. Journal of the American Psychoanalytic Association, 43, 1051-1084.
Garza-Guerrero, A.C. (1974). Culture shock: Its mourning and the vicissitudes of identity. Journal of the American Psychoanalytic Association, 22, 408-429.
Obama, B. (2017, September 5) Immigration can be a controversial topic. [Facebook update] Retrieved from https://www.facebook.com/barackobama
Volkan, V. D. (1993). Immigrants and refugees: A psychodynamic perspective. Mind and Human Interaction, 4, 63-69.
Print a copy of this article here.

Dr. Shibley is a clinical psychologist with a private practice in Banker’s Hill, where she conducts psychotherapy with adults, couples, and families. She specializes in issues around acculturation, immigration, and trauma. For the past ten years, she has been conducting psychological evaluations for individuals in immigration proceedings and works collaboratively with attorneys and legal firms throughout California as an expert witness.
Sidney Zisook, M.D.: An Innovator in the Treatment of Grief and Suicide Prevention
Interview by Erika Kao, Ph.D.
 I had the pleasure of interviewing Sidney Zisook, MD at his office at University of California, San Diego (UCSD). Filled with natural light and cozily decorated, his office is an inspiring environment for research on therapeutic mental health interventions.
I had the pleasure of interviewing Sidney Zisook, MD at his office at University of California, San Diego (UCSD). Filled with natural light and cozily decorated, his office is an inspiring environment for research on therapeutic mental health interventions.
Dr. Zisook is an accomplished researcher and Professor of Psychiatry at UCSD, and a kind, interesting, and warm person. His interest in Grief and its manifestations have roots in both his personal and professional life; he first began thinking about Grief as a teenager, when he encountered it first-hand after losing a close friend. His professional interest in Grief began when his mentors at Massachusetts General Hospital, where he was a resident, and at Harvard Medical School, where he was a fellow were studying Grief as a model for resilience or psychopathology. Today, Dr. Zisook is considered to be a leading authority in the field of Grief research.
What is “Complicated Grief” (also known as prolonged grief, or, in the DSM-5 as “persistent complex bereavement disorder”) and how does it matter to you as a clinician?
“There is no formula for how to grieve or a definition for ‘normal’ or ordinary grief. Everyone grieves in their own way: Grief may be different for different losses, and shifts over time. Yet, there are some commonalities, including intense emotionality (e.g., pangs of yearning, longing, sorrow, anxiety, guilt, anger and shame Interspersed with positive emotions), cognitions (e.g., a sense of disbelief, frequent insistent thoughts and memories of the person who died, difficulty concentrating on other things) and behaviors (e.g., proximity seeking and/or avoiding reminders of the loss). Many of these features overlap with symptoms of depression and, especially after a very violent, sudden, unanticipated or traumatic loss, such as after suicide, accidents or homicide, features that overlap with posttraumatic stress are common. Nevertheless, for most bereaved individuals, intense emotionality subsides, thoughts and memories recede into the background, the sense of disbelief lessens, and wellbeing is restored. Although the loss will never be erased, healing occurs over time and the individual is able to get on with this or her life. However, sometimes this progression gets derailed and intense grief persists, often accompanied by strong negative feelings such as unrelenting guilt, blame, and loneliness, avoidance of, or preoccupation with, reminders of the deceased, feeling disconnected to the past, present and future, and a sense of meaningless and despair. This condition, the failure to adapt to the loss, is what we call ‘Complicated Grief.’

Angel of Grief (art by Maryam Mughal)
Those suffering from Complicated Grief may have self destructive tendencies; they appear unable to move forward, and are at higher risk for suicide. In the DSM-5 complicated grief is identified as Persistent Complex Bereavement Disorder (PCMD), a condition for further study. It appears in the section of Trauma-and Stressor-Related Disorders. Complicated Grief (or PCBD) differs from Posttraumatic Stress Disorder (PTSD) in that the trigger is loss rather than threat. Correspondingly, primary emotions are yearning and sadness rather than anxiety and fear. Intrusive thoughts and images are focused on the person rather than the event, and these thoughts and memories are not frightening. At times, they may even be pleasurable.
In the absence of treatment, Complicated Grief may persist indefinitely and is associated with substantial ongoing emotional pain and psychological and medical morbidity. The good news is that there are several emerging, evidence-based therapies for Complicated Grief. The form of therapy with the most evidence, simply called Complicated Grief Psychotherapy (CGT) has now been found effective in three large, randomized trials. CGT is a form of cognitive behavioral therapy that also draws upon exposure therapies, interpersonal therapy, motivational interviewing and gestalt therapy. Each of the 16 manualized sessions focuses on both loss and restoration.”
A recently completed NIMH-funded randomized controlled study of CGT lead by Dr. M. Katherine Shear (Columbia University) with Drs. Charles Reynolds (University of Pittsburg), Naomi Simon (Harvard), and Sidney Zisook (UCSD) also explored the role of antidepressant medications for symptoms of Complicated Grief. That study did not find medications particularly effective, either alone or in combination with CGT, but it did confirm the robust effectiveness of CGT. At the initiation of treatment, participants had been profoundly impaired, often for several years. Comorbid depression and PTSD were common and 43% of the bereaved participants expressed suicidal thoughts at the start of treatment. Despite the severity and chronicity of symptoms, an impressive 83% of the treatment group responded to CGT. There were corresponding improvements in function, depressive and anxious features, and suicidality. Indeed, none of the participants who received CGT were suicidal at the end of treatment. In addition, the subset of participants who had suffered from losses that were particularly violent and traumatic, such as after suicide, accidents and homicide, did equally well with CGT as those whose loved ones died from nonviolent, natural causes of death. Few clinicians are familiar with this innovative and highly effective treatment, and thus may not well equipped to optimally help their clients with Complicated Grief.
Dr. Zisook also shared important work he has done in suicide prevention. He is involved in a project to reduce suicide amongst physicians and other healthcare providers. Healthcare providers, including physicians, nurses, and pharmacists are at elevated risk for suicide (there is anecdotal data that psychologists, too are risk for suicide, but there are no studies yet). Female physicians are at especially at high risk. In light of these sobering occupational risks, Dr. Zisook and his team at UCSD have launched a proactive educational, support and outreach program aimed at destigmatizing mental health treatment, and preventing burnout and suicide.
Dr. Zisook, Alana Iglewicz, M.D., and Danielle Glorioso, L.C.S.W. of the UCSD Complicated Grief Study Team will talk about this ground breaking treatment for Complicated Grief at the SDPA Fall Conference taking place on October 28th, 2017.
Print a copy of this article here.

Dr. Kao has been a licensed psychologist since 2001. She practices in the Del Mar- Carmel Valley area. She has two sons, and a small but fearsome dog. Attachment theory in relationships, career development, anxiety, trauma, grief, loss, and medical/legal assessment are her areas of practice.
A Storm Can Change the Balance
Poem by Mark W. Stevens, Ph.D.


Art by Claude Vernet
Print a copy of the poem here.
Editor’s Note: Please look out for Dr. Stevens’ essay in the next issue of The San Diego Psychologist about his experiences with the Red Cross disaster relief for the victims of Hurricane Irma.

Dr. Stevens is a clinical psychologist, and currently has a private practice in Poway, California. He has previously practiced in Hawaii. He is married and has six daughters. When not working, he enjoys music, hiking with his wife, painting and drawing, and writing short stories, poems, and novels.
President’s Corner
by Annette Conway, Psy.D.
Welcome to the Spring 2017 issue of the San Diego Psychologist!
My beginnings in clinical practice were a time of trial and error, as beginnings often are. Early in my career, I had not established whether (and at what point in therapy) to include the partner or family of an individual client. When I did encourage my clients to bring significant others or family members to session, they would show up with their spouse, mother, father, maybe a brother, and so on. My most memorable experience from those early days is about a Latino client, to whom I implored at the end of a session, “Por favor come in with your family”. The next week, imagine my surprise when I saw that the gentleman had arrived with 23 members of his family!
I learned two important lessons on that fateful day: that I needed to have more structure in my therapeutic process and that family is a vital part of treatment. In my 20 years of practice, I have worked with many, many clients, and the one thing I keep coming back to is the value of treating the client in the context of his or her family, rather than as an autonomous individual.
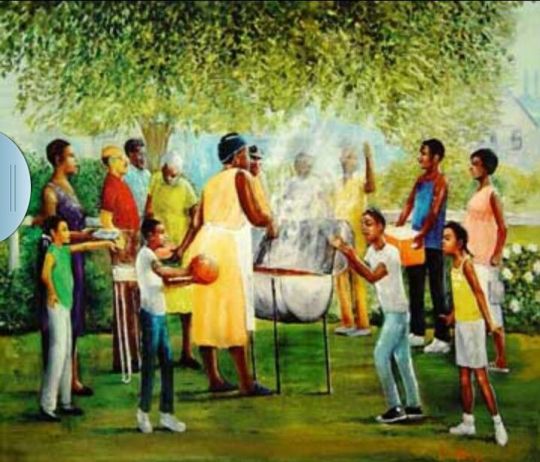
Artist Unknown (Sourced from Pinterest)
I am pleased to focus this issue of the San Diego Psychologist on Couples and Family Therapy. Research shows that Marriage and Family Therapy is as (and in some cases, more) effective than Individual Therapy, in that it facilitates the change in patterns created by the family system. For clinical reasons, couples and family counseling gives the therapist an opportunity to conduct a thorough biopsychosocial assessment of the couple or family needs. Valuable information regarding family dynamics, coping abilities, communication skills, social relationships, and conflict-resolution skills, in addition to the individual client’s self-report can contribute to a more accurate case formulation and therefore, a more appropriate treatment plan. In addition, how the therapist “experiences” the couple and/or family supports or questions organizational abilities, boundary fluidity, cultural and religious customs, and daily rituals of the client.
As you read this issue of the San Diego Psychologist, we want to remind you of SDPA’s full-day conference on cutting-edge issues and up-to-date information on complex issues facing youth, families and communities, in collaboration with The California Association of Marriage and Family Therapists, San Diego Chapter, The San Diego Academy of Child and Adolescent Psychiatry, and the San Diego Psychiatric Society. It has been exciting working closely with our allied professional associations to provide this valuable educational opportunity to clinical practitioners, educators, behavioral health, and child welfare and community organizations in San Diego County.
The CICAMH collaborative also sponsors a Free Networking Event every August at a local brewery. This year’s Summer Networking Social is scheduled for Sunday, August 27, 2017, 3:00pm – 6:00pm at Stone Brewery, Liberty Station 2816 Historic Decatur Rd #116, San Diego, CA 92106.
Register at: https://goo.gl/forms/7WKcxD22RYLHo7jQ2
It is a great opportunity to connect with other individuals with the purpose of enhancing professional and social networks, in addition to learning more about community resources. I hope to see you all there!

Dr. Conway is a clinical psychologist in private practice and the President of the San Diego Psychological Association
Editorial
Dear SDPA members and guest readers,
Welcome to the long-overdue issue of the San Diego Psychologist. Clearly, we are well into summer, but the reason for this delay is that we had no content for our issue by the original May 31st publication date. Simply put, we did not receive a single response to our call for articles. The articles that comprise the current issue with the theme of Couples or Family Therapy were directly solicited from the authors, identified as experts in their respective fields.

As clinicians, we know the importance of alliance building, perceptiveness and intuition, and the ever-changing dynamic between the self and other in any therapist-client dyad. These parameters become much more complicated when the therapist has to maintain an alliance with the couple or family as a unit while balancing an alliance with each member of the unit, and at the same time, helping them navigate through and resolve their conflict. The therapeutic process is a delicate dance that demands a special set of skills on the part of the therapist.
Each of the five articles in this issue presents either a challenging problem relevant to couples or family therapy, a focus on therapy with families from minority or underserved populations, or both. Ms. Estes, a licensed marriage and family therapist specializing in working with clients from the LGBTQ community and ethnic or cultural minority groups has written a thoughtful article providing basic guidelines for therapy with these highly underserved clients. Dr. Wexler, a clinical psychologist and chair of the SDPA Fellows Committee has drawn from his decades of working with couples in conflict to present his fascinating essay on helping nurture intimacy in relationships. Dr. Spring, a nationally acclaimed expert clinician and author on helping couples navigate infidelity; she will be headlining the conference on Sex and Relationships at The Relationship Training Institute in San Diego this November. Mr. Witter, a licensed marriage and family therapist has focused his article on one of his specialties, i.e., working with emotionally escalated couples. He has artfully described his use of Emotionally Focused Therapy in guiding these couples through their emotional pain and insecure attachment to a place of safety and security. Last but not least, Dr. Falicov, an internationally heralded clinical psychologist specializing in working with immigrant families has described two case examples highlighting common issues that can create conflict between immigrant couples. She describes her culturally-sensitive therapeutic process while never losing sight of the developmental cycle of couples that pervade all cultures.
I sincerely hope you learn as much from this issue on Couples and Family Therapy as I did. Our next issue, which will be published in late summer, will focus on the urgent and current topic of mental health in the current political climate. The topic was unanimously selected by the SDPA Board, in the hope that there are enough of you who feel passionately about writing about your experiences and thoughts regarding this tumultuous time in our nation’s history and its emotional fallout. The submission deadline for the Summer 2017 issue is August 1st. Please help us make this issue a success with your contributions.
Please share your feedback in the comments below, or email me at TheSanDiegoPsychologist@gmail.com.
Thank you for reading.
–Gauri

Gauri Savla, Ph.D. has been the editor of The San Diego Psychologist since January 2016. She is a clinical psychologist in private practice and specializes in geriatric mental health.
What to Consider When Working With Underserved Populations
by Jennine Estes, LMFT
Have you ever worked with a client who was the victim of a brutal beating because he was gay? Or has a client ever shared with you that they have been shut out of a community simply because of their skin color? Has a client resisted opening up to you out of fear that you won’t understand their religious orientation? These are real cases and situations that are all too common with underserved populations. The specialized mental health training and education required to properly help this group cannot be emphasized enough.
Definition of an underserved population
Underserved populations are groups of minorities, such as same-sex couples, ethnic minorities, the physically impaired, polyamorous relationships, and refugees. They face both daily struggles and lifelong challenges that impact them emotionally, physically, psychologically, and financially.
For example, in my group practice, we work specifically with the LGBTQ (gay, lesbian, bisexual, transgender, and queer) population and help our clients process and address the various layers of discrimination, hate attacks, family rejection, shame, and isolation that they have been through or will face.

Artist Unknown (Sourced from Pinterest)
Considerations when treating underserved populations
As mental health professionals, it is our responsibility to be educated on the specific struggles of underserved populations and consider how we can best address them. This may include approaches that are unique to any other client population you deal with.
The first area to consider when working with a minority client is to be aware that there may be layers of pain. Each client can emotional scars, but the underserved group has additional scars that are different in the sense that they have seen negative impacts on their education, career, place of residence, family, and more.
This group has not typically had space to talk about their experience, often being shut out because these experiences are not part of traditional social norms. For example, the LGBTQ community is commonly known for being “closeted,” having to disown parts of who they are and starting as early as childhood. Shame grows rapidly when disowned parts are kept in the shadows, unspoken. Furthermore, when society sends additional shaming messages, the corresponding pain increases. In relationships, the history of being open or closed about their sexual orientation impacts the security in the relationship. Couples can often draw close to one another, sharing similar experiences and understanding one another. At other times, a partner may struggle with the degrees of their openness which impacting the security in the relationship. In short, underserved populations carry pain, and it must be recognized.
Secondly, know that discrimination and the fear of discrimination is real and alive. For example, the Orlando nightclub shooting resulted in the deaths of 49 people in a gay club, and is one of the many hate attacks that keep people fearful for their safety simply because they are in a same-sex relationship. Another example of how clients are impacted is by the history of African American slavery and the current legacy of discrimination resulting from that.
My team of therapists works with LGBTQ clients and clients of color who have experienced hate attacks that range from public verbal abuse to being beaten to the point of hospitalization and fighting for their life. Even though we are in 2017 and live in San Diego, a city that values equality, it is still important to understand your client’s trauma history and to know that your client’s fear of discrimination is alive and real; they will always be scanning their environment to assess if the space is safe.
In a couple, the fear of social discrimination impacts the relationship on various levels. If one partner withholds their affection, it sends a message as if they don’t care or not proud of the relationship. The lack of communication around the discomfort can leave the other partner feeling in the dark and taking it personally. Other times, couples can come together and connect on their experiences.
Third, realize your clients’ decisions for the future are impacted by their religion, skin color, or sexual orientation. For example, a lesbian couple planning on having a child will reconsider where they should live to ensure their child will be safe and accepted in the neighborhood. Or a Hispanic couple moving to an all-white school district will worry about how to help their child fight discrimination.

Artist Unknown (Sourced from m.Favim.com)
What we can do to help our clients
First, there is no better way to help your clients than to talk about it. Ask the questions. Lean in to the uncomfortable topic of religion, ethnicity, or sexual preferences. Create a safe space for them to open up, because some people likely haven’t had that before. The more they talk about the rejection, physical and verbal attacks, and discrimination they’ve encountered, the more power they have. We need to help our underserved clients process their experiences so they don’t remain cloaked in shame.
Secondly, help them own all parts of themselves: their skin color, sexual orientation, religion, etc. Empowering our clients to feel proud of who they are will help combat the shame, embrace their community, and acknowledge the courage and strengths they have.
Next, address the inevitable feelings of loneliness and isolation. For example, transgender clients and their families often feel very alone, so connect them to groups where they can share stories and support one another. Encourage your clients to seek out their community either face-to-face or online. Supportive communities are out there; your clients just need the help knowing that those connections can be healing and are an important part of feeling more confident in their own skin.
Finally, even though San Diego is very open-minded compared to other cities across the country, there are still violent crimes geared toward race, sexual orientation, and other minorities. Better yet, they may experience rejection by their own family and friends. Help your client with setting boundaries. This includes developing a situational awareness and determining where it is safe to take their armor down and where they must keep it up. Encourage your clients to get educated when traveling to foreign countries knowing where it is safe versus unsafe for them to go.
In conclusion, underserved populations are impacted by the past, present and future. Their emotional and psychological scars influence how they connect with peers and loved ones, seek job opportunities, and engage in their communities. By getting trained and educated on the struggles underserved populations face, we can help them through the challenges, enhance who they are, and help them have a voice.
Print a copy here.

Jennine Estes is a Licensed Marriage and Family Therapist and certified in Emotionally Focused Therapy. She is the owner of Estes Therapy, a group practice working with couples and individuals using EFT and EMDR. She has an online relationship survival guide called Relationships in the Raw and a #BeingLOVEDIs campaign that connects directly with the community.
The Path of Intimacy
by David B. Wexler, Ph.D.
When I see a couple for the first time, I usually open with a good old-fashioned, open-ended question to get the ball rolling: “What are you doing here?”. I pay close attention to their opening line in response, i.e., “the headline story.” Often, it is clear that they have thought about this carefully, and the first answer to this question tells me exactly what our project is going to be together: “I have a drinking problem and it’s killing our marriage,” or “It just seems like we have drifted apart,” or “My husband found out that I have been seeing someone else and he can’t forgive me.” Less often, I get a vague answer that doesn’t tell me much, typically, and “We have a problem with intimacy.”
I never presume what “having a problem with intimacy” means to these particular two people. Are they not having sex? Are they having sex but not enjoying it? Are they not speaking to each other? Have they drifted into leading separate, distant, parallel lives? Do they not feel safe and trusting with each other, thus blocking intimacy? Is someone having an affair? Does it seem like they just don’t like each other very much? Over the past quarter century of working with couples, I have heard enough of these statements and discovered the true meaning behind them, which has led me to develop a map of the multiple components of an intimate relationship. I call these components the Four Pillars of Intimacy.
What does healthy intimacy look like?
The healthy, vibrant, loving, trusting, connected, self-actualized relationship rests on the Four Pillars. When these pillars are shaky or collapsing, the structure they hold up collapses as well. Not every couple has all of these pillars in great shape, but there is a direct correlation between the strength of these pillars and the healthy intimacy they experience. No one pillar is any more important than the others; rather, they create a synergistic effect.

Source: http://crushedgrapesnddreams-blog.tumblr.com/post/66203633112
The first pillar is Safety & Security. No relationship has a fighting chance of true intimacy if one or both partners do not feel safe. Intimacy requires vulnerability, and vulnerability requires safety. Physical safety is paramount, in that, any threats of violence are totally incompatible with intimacy. Similarly, the relationship needs to be free of lies and deceptions, as well as threats of abandonment, humiliation, and betrayals, i.e., there needs to be emotional safety and security. If your partner is emotionally or physically threatening, or emotionally or physically unfaithful, or fundamentally not to be trusted to refrain from deeply hurting you, how can you be intimate?
The second pillar, Knowing & Being Known, refers to the ways in which both partners truly know each other. Even if you feel reasonably safe, you are not likely to experience intimacy unless you really know each other. The rewards of truly knowing another and truly being known by another are enormous. This goes beyond knowing details of your partner’s life; it also includes knowing about his or her inner world, vulnerabilities, fantasies, dark places, and wonderful places. Knowing leads to empathy, which leads to genuine acceptance, which in turn paves the way for true intimacy. Some couples have this naturally, some need to work harder to enrich it, and others never achieve it.
The third pillar is Affection and “Likeability.” These qualities contributing to intimacy show up in multiple venues: physical touch (non-sexual), non-verbal cues (like smiling), verbal statements (like “I love you” or “I’m so proud of you”), and generous behaviors or gestures (like bringing someone a cup of coffee or laughing at their jokes). When this area of a relationship is thriving, both parties feel consistently and genuinely liked by the other. The joys and rewards of feeling genuinely liked help people withstand the inevitable assaults and dissatisfaction in the course of any normal relationship.
The fourth pillar, Passion, Chemistry, & Sex, is the most complex. The other three pillars are, more or less, receptive to conscious effort and creative manipulation if the individuals are truly motivated. Passion, chemistry, and sex are more difficult to consciously generate. Many couples who have at least moderate levels of attraction may lose that connection, and the strategies for generating more passion often rest on making sure that the other three pillars are solidly constructed.
Why can’t we all just get along?
There are only three reasons why intimacy gets complicated. And the story you tell yourself about why you are struggling with intimacy, or why your partner is, can make all the difference in the world.
Reason #1: Pure Fear
For a thousand reasons, we carry fears associated with intimacy. We feel vulnerable. We are afraid of being hurt, rejected, abandoned, humiliated, or betrayed. Everyone is afraid, but some of us are more afraid than others, almost always because of experiences growing up that have shaped us, consciously or unconsciously.
Reason #2: Cluelessness
Another reason that often complicates intimacy is gender-specific intimacy behaviors that backfire; men, in general, have not been sufficiently schooled in the art of empathic communication with women. Women often seek verbal intimacy in ways that may alienate men. Many men confuse the intensity of sexual intimacy with the big picture of full intimacy and seem mystified when their female partners seem uninterested, turned off, misunderstood, or disrespected. Women often try to be “helpful” by offering excessive suggestions or interpretations of their male partners’ behaviors, who may perceive that behavior as controlling or maligning.
Reason #3: Not Caring and/or Burned Out
If you are in this category, don’t bother reading this article because it will not help you. You may “suffer” from a personality disorder of psychopathy, or your “dismissive attachment” may have shut you down so profoundly that you have permanently given up on the possibility of human intimacy. You may be missing a chip for normal human interaction.
If you are in a relationship with someone like this, my best advice is to get out.
Why bother with nurturing/enhancing intimacy?
This might seem like a rhetorical question to those among us who naturally crave intimacy in all its forms. But to those who are conflicted about intimacy or are reluctant to engage in the rituals that seem to enhance intimacy, here are some good reasons to reconsider that reluctance:

Artist Unknown
Intimacy feels good: Attachment stimulates vasopressin and oxytocin, the “bonding” chemicals in our brains. People who have lived a long and rich life consistently attribute their emotional well-being to relationships, rather than accomplishments.
It usually beats the alternative: The alternative to experiencing genuine intimacy is loneliness and alienation. Some people who consistently fail at intimacy may decide that pursuing it is not worth the pain of failure. Rarely do these people express mental well-being and contentment from life. It must be acknowledged that nurturing intimacy in relationship can be demanding. Commitment comes with loss and conflict and vulnerability, and in rare cases, even even trauma.
Intimacy can facilitate the resolution of other relationship issues:: When there is a solid foundation of intimacy, every other relationship bump in the road remains a bump in the road and nothing more. It is easier to listen. It is easier to accept criticism. It is easier to bounce back after spats and hurt feelings. It is easier to accept dull periods, losses, disappointments, frustrations, sexual deprivation, sexual rejection, differences on vacation preferences, disputes about child-rearing philosophies, and everything else.
Intimacy helps cope with loss: Researchers on midlife transitions and the psychological aspects of aging identify the inevitable losses involved as we move through different life stages. But one quote about this process that I often pass on to couples offers tremendous perspective and tremendous hope: Real intimacy diminishes “the narcissistic sting of aging” (Colarusso, C. A., & Nemiroff, R., 1981). The “sting” may refer to changes in physical appearance, or the realization that we have been imperfect parents or friends or workers. But he rewards of genuine, seasoned intimacy, the kind that can only develop over time on the mutual and emotionally raw ride through good times and through bad, provides a profound buffer to this “sting.”
Real intimacy often leads to more and better sex.
Last but not least, for most of us there is no more powerful way to genuinely grow as a human being: The brilliant psychiatrist and psychoanalyst C. G. Jung once said: “One is always in the dark about one’s own personality. One needs others to get to know oneself” (Jung, C. G., & Hull, R. F. C., 1977).
There is nothing that gives you the opportunity to know who you really are more than a truly intimate and authentic relationship. Intimacy is not limited to lovers. The unparalleled personal growth opportunities from intimacy can also be generated in your relationships with your children or parents or perhaps a few select others. If you needed even one more reason to really dig for intimacy, this is it: a purely selfish one.
Print a copy here.

David B. Wexler, Ph.D. is the Executive Director of the Relationship Training Institute (www.RTIprojects.org) and the author of six books, including When Good Men Badly, Men in Therapy, and The STOP Program for Domestic Violence. dbwexler@gmail.com
Secrets, Cybersex, Infidelity, Addiction, Trauma…and Forgiveness?
by Janis Abrahms Spring, Ph.D., ABPP
After an affair is discovered or revealed, an emotional avalanche is triggered that is often difficult for both patients and therapists to control. In my workshop with the Relationship Training Institute on November 10th, 2017, I will help therapists help their patients reframe an affair as a psychological trauma, learn how hurt and unfaithful partners respond differently to an affair, appreciate how this difference can promote healing, and learn how partners can make a healthy, self-interested decision regarding reconciliation. I will also present concrete strategies for rebuilding trust and sexual intimacy after an affair.
Infidelity is defined as a violation of sexual exclusivity when a spouse has sexual intercourse with someone other than his or her partner without that partner’s consent. But this definition is strictly limited to married (heterosexual) couples and sexual intercourse. Besides including other types of committed relationships, we need to broaden the definition of infidelity to factor in Internet sex. People are spending hours talking intimately with others they will never meet, let alone touch. However, when committed partners learn of this betrayal, they often feel severely violated and decimated. As a general rule, if your partner were in the room looking over your shoulder feeling very uncomfortable with what you were doing, that may constitute an affair. At their core, affairs are about secrets and the violation of trust.

Artist Unknown
Today, there is a new world of affairs in the domain of cybersex. One of the great attractions of Internet affairs is that you can be anyone you dream of being. You can pretend you are a priest when you are a criminal, a man when you are a woman, and so forth. Often the attraction of an affair is not to the lover per se; that person may be someone the unfaithful partner idealizes or barely knows. Rather, the attraction is to the experience of the self – and that experience of romantic love, of transcending one’s personal limitations, can be quite transcendent and emotionally convincing. To reiterate a point I have made in my previous writings, not only can the hurt partner not compete with the fantasy of the affair person (i.e., the unfaithful partner’s lover), but the affair person cannot compete with the fantasy of the affair person. Fantasies usually promise more than we get in real life. Before unfaithful partners give up on their spouses for someone they barely know, they should ask themselves to name five things they know they will be fighting over with the affair person.
In my first book, “After the Affair: Healing the Pain and Rebuilding Trust When a Partner has been Unfaithful,” I propose a three-stage model for healing.
The first stage is making sense of the trauma of infidelity, i.e., giving a language to its effects and helping partners normalize what they are experiencing. The second stage is making a thoughtful, not an emotional, decision about whether to stay together. The third stage is for those couples who choose to stay together and learn lessons from the affair which will strengthen their bond. Here, I suggest practical strategies for how to rebuild trust, rekindle sexual intimacy, and grant or earn forgiveness in ways that make it human and attainable.
Making sense of the trauma of infidelity
Let us begin with the emotional response of the hurt party. When hurt partners discover their partner’s affair, they experience a post-traumatic stress-like reaction in which two simultaneous and competing responses occur: hyper-arousal and deadening. On the one hand, they may find it difficult to concentrate or sleep, their minds often bombarded with images of the lover. At the same time, they may lose interest in everything that used to give them meaning or purpose.
Hurt partners often describe nine types of psychological losses, described below:
- Loss of identity: You cannot recapture the way you are used to knowing yourself. For example, if you once thought of yourself as zesty, attractive, and capable, you lose all sense of your familiar self after discovering your partner’s affair.
- Loss of specialness: You thought that you could make your partner happy the way no one else could, and you now realize that you are disposable and interchangeable.
- Loss of self-respect: Hurt partners often go to extreme measures to win their partner back and feel humiliated by their desperate behavior.
- Loss of self-respect for not acknowledging that you were wronged: Often the cues of deception are obvious, but hurt partners don’t confront them because the truth is too shattering. They are left struggling to forgive themselves for not speaking up about violations in the relationship.
- Loss of control over thoughts and actions: Often, hurt partners become obsessed with details and spend hours compulsively checking for information.
- Loss of a sense of order and justice in the universe: There is a sense that the world no longer operates according to specified rules, instead, is arbitrary and cruel.
- Loss of religious faith and belief in a higher power: “If God were good,” hurt partners ask, “why would He do this to me? If I were good, why would this happen?”; the hurt partner’s sense of alienation and loss of self-confidence are profound.
- Loss of connection with others: Whom do hurt parties turn to? They often want to tell their family and friends but recognize the awkwardness or destructiveness which may follow.
- Loss of a sense of purpose and the will to live: This is an extreme reaction to the affair and can be fatal.
These losses capture the deep and pervasive sense of betrayal, which hurt partners experience when the affair is revealed. The most important strategy for therapists is to get patients to talk about and appreciate their losses. They will be embarrassed to admit how “badly” they believe they are coping. By giving their experience a name and context, however, therapists have a chance to help them feel less crazy, helpless, and alone. This normalization may be the most significant healing gesture therapists can offer their hurt clients.
What about unfaithful partners? Their response to the affair often is quite different, which is one reason why this work is so challenging. As eviscerating as the affair is to hurt partners, it is often validating and expansive for unfaithful partners.

Artist Unknown
Let us look at some of the more common emotional responses of unfaithful partners. Often their first response is relief. They may be relieved that their secret is out in the open. Next, they are often impatient; they want to move on. But to move on, they must learn to pay attention to their partner’s pain. In my book, “How Can I Forgive You? The Courage to Forgive, The Freedom Not To,” I talk about how therapists need to help unfaithful partners create “a transfer of vigilance.” That means, unfaithful partners must approach their partner’s trauma, express remorse, and talk about the lessons they have learned about why the affair happened. They need to address those issues that made them vulnerable to an affair, work to earn trust, and make their partner feel loved and cherished.
At the same time, hurt partners may need to learn to let go of their preoccupation with the injury, and to not bring it up every time they think of it. They also need to take a fair share of responsibility for how they may have created space between them and their partner to allow a third person to come in between them.
Other responses of the unfaithful partner include grief over the loss of the lover, justified anger and the absence of guilt, fear of losing the love of their children, paralysis (the inability to decide whether to end their relationship with the affair-person or marriage partner), and self-disgust.
Both partners need to learn how to manage their fears. The greatest fear of the unfaithful partner often is that they will never be forgiven no matter how hard they work to rebuild trust. The greatest fear of the hurt partner often is that they will never feel safe or that they will continue to turn up evidence that renders them insecure. This belief makes it hard for unfaithful partners to recommit.
Making a thoughtful, rather than emotional decision about reconciliation
The second stage of recovery from an affair requires both partners to make a thoughtful, not an emotional, decision about whether to reconcile. This is a two-step process: making sense of feelings of love, and directly confronting one’s ambivalence about returning home. When it comes to feelings of love, both partners may struggle with an intense but unwarranted attachment, i.e., the hurt partner’s love for their partner, and the unfaithful partner’s love for the person they had an affair with. Hurt partners may love a partner who is incapable of meeting their essential needs. Unfaithful partners may feel romantic love for the lover and be willing to risk everything for someone they hardly know. They may need help understanding the emotional, cognitive, and chemical underpinnings of romantic love so they don’t act precipitously and toss away a potentially salvageable relationship with their committed partners.
In deciding whether to recommit to the marriage, partners should be encouraged to express their doubts and fears. Therapists can then help partners respond in a thoughtful way. Typically, partners may wonder, “Yes, you’re making changes, but are they permanent or sincere?”; “Do you want me or just the package?”; “Should I stay for the sake of the children?”; “If I spend more time with the lover, might I be able to make a better decision about what is best for me?” and, “after so much damage has taken place, how can I trust you again?” These questions underscore each partner’s ambivalence about recommitting and must be answered thoughtfully.
Rebuilding the relationship
After an affair, there are three essential conditions to rebuilding trust and earning forgiveness. Unfaithful partners must 1) pay attention to the pain they caused and offer a meaningful, generous, specific, heart-felt apology, 2) they must look deeply into themselves and figure out why they strayed so they can protect the boundaries of the relationship, and 3) they must work hard to earn trust and generate feelings of love. Both partners need to take a fair share of responsibility for how they contributed to creating a space between them that made room for someone else, and to work hard to make their partner feel loved and cherished.
Those who attend this course will hear my unromantic model of love and reconciliation. It begins when the unfaithful partner has a funeral for the lover and, turns toward the hurt partner. Then both partners begin to treat each other in ways that foster tenderness, trust, and intimacy. And then, last (not first, as many partners wish), feelings of love may return.
Print a copy here.

Dr. Spring is a nationally acclaimed expert on issues of trust, intimacy, and forgiveness. She is author of the award-winning How Can I Forgive You? The Courage to Forgive, The Freedom Not To; After the Affair: Healing the Pain and Rebuilding Trust When a Partner Has Been Unfaithful, and Life with Pop: Lessons on Caring for an Aging Parent. In private practice in Westport for 40 years, Dr. Spring is a recipient of the Connecticut Psychological Association’s Award for Distinguished Contribution to the Practice of Psychology and the Connecticut Association of Marriage and Family Therapists Award for Distinguished Family Service. Board Certified in Clinical Psychology, she is a former clinical supervisor in the Department of Psychology at Yale University. www.janisaspring.com
Emotionally Focused Therapy for Emotionally Escalated Couples
by Ian Witter, LMFT
Sarah and Robert have been married for five years. When scheduling the appointment, Sarah tells you that they’ve been having “communication difficulties.” During the first session, Sarah states that they have been arguing and that the arguments can get pretty nasty. She elaborates, saying that she feels attacked, and blamed for the distress in their relationship, and that she perceives Robert as having an anger problem. Robert, who was sitting quietly up to this point explodes with, “I wouldn’t get so angry if you weren’t such a nag!” Sarah responds with “This is exactly what I was talking about, I don’t know why I even try! Why do you have to be such a dick?!” Robert responds with another derogatory statement about Sarah’s character, and you, the clinician, are left wondering about career options at Starbucks. What causes these seemingly out-of-control outbursts among couples? What can you, as their clinician do to help slow them down and get them to a place of safety and connection?

Pencil Sketch by Brigid; http://burdge.tumblr.com/tagged/my+art
For clinicians who work with couples, such “escalated” couples can be the most daunting of cases. These are the couples who come to therapy seeking assistance, but frequently end up engaging in yelling matches, during which they seem more interested in name-calling and making threats than working on their relationship. As a clinician who specializes in Emotionally Focused Therapy (EFT) in my work with couples, I appreciate the challenges posed by taking on escalated couples as clients and understand why many clinicians refuse to work with them. Escalated couples can make us question our skills as a clinician, and push our buttons personally. Fortunately, EFT was created to work with clients experiencing distress in their relationship, and can be very effective in working with highly escalated couples. For those unfamiliar with the EFT model, here is a brief overview.
EFT is a systemic, evidence-based approach to couples therapy, based in attachment theory. Its underlying assumption is that every individual longs to find a sense of belonging, safety, and acceptance with at least one other person in his or her life. This seemingly innate need for attachment to another exists across socioeconomic classes and cultures. But what happens when the interactions with our partner doesn’t feel safe or secure? How do we respond to this relational stress? Couples with an insecure attachment to one another can respond with defensiveness, anger, blaming, and accusations, or distancing and withdrawal. Common manifestations of relational distress include infidelity, substance use, or physical or emotional abuse. EFT views these negative responses as a reaction to perceived abandonment and a fracturing of the desired secure attachment by a partner. By putting these responses in the context of heightened emotional need, EFT helps couples reframe these negative emotional responses as a desire for safety and security. This is done by helping the couple recognize their primary emotions and how these are connected to the underlying attachment needs of each partner. EFT is also experiential, i.e., part of the therapeutic process is to structure new conversations in which the couple can communicate these attachment needs. In short, EFT helps to drive connection through emotional vulnerability as opposed to emotional reactivity.

Pencil Sketch by Brigid; http://burdge.tumblr.com/tagged/my+art
EFT also views negative interactional patterns within a distressed relationship as consistent and predictable, regardless of the content of the argument. Each partner’s relatively predictable relational role is usually related to their underlying attachment style (secure, avoidant, or anxious). As clinicians, how many times have we heard one partner say, “I can never get anything right, so now I don’t even try” (avoidant attachment style) and the other state, “I feel like I’m all alone in the relationship, and that my partner doesn’t care about my feelings at all” ( anxious attachment style). The typically avoidant tend to withdraw into themselves in times of stress. The typically anxious tend to find comfort through interactions with another, and when they don’t get comfort, can become critical and blaming in their attempts to find it. When one partner creates distance and avoidance, and the other craves closeness and intimacy, trouble results. EFT recognizes this pattern as the “cycle” that occurs for distressed relationships, regardless of the content of the communication.
EFT is comprised of three stages and nine steps. The typical course of treatment is 8-20 sessions, but underlying issues (trauma, substance use, infidelity) affecting the relationship can extend the length of treatment.
Stage One: Assessment and de-escalation of current negative cycle
Step 1: Create alliance with couple and assess issues that create conflict, with a focus on how these issues are related to the underlying attachment issues for each partner.
Step 2: Identify the negative cycle, and each partner’s position in that cycle. Focus on each partner’s behaviors, thoughts, secondary and primary emotions, and unmet attachment needs.
Step 3: Access underlying emotions both partners feel in the course of the negative cycle. Hearing their partner’s relational experience attached to other vulnerable emotions instead of rigid negative emotions helps to temper their own interactional patterns.
Step 4: Reframe the presenting relational conflict in terms of unmet attachment needs and primary emotions. Frame the negative cycle as the source of the relational distress, thereby externalizing the cycle they experience.
Stage Two: Changing interactional process; restructuring emotional bond between partners
Step 5: Foster identification of previously disowned aspects of self (emotions and attachment needs) and integrate these into relationship by sharing with the other partner. Identify how these disowned emotions have prevented the partner from reaching out authentically.
Step 6: Promote acceptance of the sharing partner’s experience, with the goal of each partner believing and trusting what the other partner is sharing, particularly, that partner’s underlying emotions and attachment needs.
Step 7: Help facilitate the authentic expression of attachment needs driven by primary emotions directly to one another, so as to dispel the old negative relational pattern.
Stage Three: Consolidation and integration
Step 8: Facilitate new solutions to old relational problems. Given the new pattern of relating to each other, it is easier for the couple to create new dialogues around previous topics they found difficult.
Step 9: Consolidate new relational positions and emotional engagement with one another.
Using these nine steps, EFT restructures the attachment bond between partners, and moves them from a place of functioning independently to functioning from a place of security. Being able to feel as if they are being experienced by their partner from a secure place helps resolve any lingering attachment injuries from childhood. Successful completion of EFT is an effective way of healing from traumas experienced in childhood or from previous relationships.

Pencil Sketch by Brigid; http://burdge.tumblr.com/tagged/my+art
Structurally, working with highly escalated couples is no different from working with less-escalated couples. In both cases, partners feel that they are unheard and alone, and are protesting what they perceive to be an emotional abandonment. The only difference is that the escalated couple is more verbally critical about it. Many individuals who are so quick to “go on the attack” have experienced what we would call “little t” trauma at some point in their history. While not enough to cause symptomatology associated with Trauma, the injuries experienced in their past are enough to cause an extreme defensive reaction in times of relational stress. These individuals are more likely to externalize what they perceive to be the source of their distress, in this case, their partner. Because they are so quick to escalate, it can be difficult to remain focused on their underlying emotional needs, and to recognize that these moments of distress are the moments in which they most need connection with their partner.
The following are some pointers to help clinicians stay connected and focused when working with highly escalated couples:
- During the course of treatment, you may become the focus of either partner’s anger. If this occurs, remember that the expressed anger is directly correlated with to the pain of being in a distressed relationship. It can be difficult to remain focused on the underlying emotional pain that a client is experiencing when their defensiveness is directed toward you. Notice that they are becoming reactive because you are touching on the place of their emotional injury – the place where they need support and validation the most. Also keep in mind that their negative response would be no different with a different therapist, working with a different model. The best approach is to validate their emotions and empathize fully.
- Be patient. These couples are often locked into these negative cycles for years. It will take time, patience, a willingness to meet the couple where they are, and persistent validation to help them begin to de-escalate. Continue placing their defensiveness and anger into the cycle.
- Be directive. When highly escalated couples first come in, it is imperative that they speak to you and not to each other. In the beginning, you need to gather information about the negative cycle between them. Letting them speak to each can be like putting a match to gasoline in that they will quickly fall into their negative cycle. Stress that they might hear something from their partner that they disagree with, but emphasize that you need to understand both sides of the relationship.
- Learn to recognize the non-verbal cues indicating your client’s reactivity, especially by watching the non-speaking client. Examples include a tapping foot, crossed arms, an eye roll, etc. To be able to say to them, “I know that what Robert is saying is upsetting you, Susan, and you may disagree with what he is saying, but it is important for me to hear how he makes sense of what is happening between you two. I also want to hear how you make sense of this place in which you two find yourself” can be enough to mollify any angry attacks. Remember, their underlying emotional experience is probably hurt, sadness, fear of being abandoned (anxious response), or feeling incompetent, and that they are failing as a partner (avoidant response). Your job is to help them recognize this and be able to share this with one another.
RISSSC (elaborated below) is one of the primary “tools” employed in EFT in order to help clients feel heard and validated. RISSSC helps clients to slow down and engage with their emotional processes rather than their defensive, cognitive processes. It also helps them to stay focused on the emotional content rather what they feel is ‘wrong’ with their partner.
Repeat: repeat key words and phrases. “It’s scary. It’s scary to think he won’t be there for you. It’s scary to feel alone and abandoned in this relationship.”
Images: use of images that have emotional content. “You feel shut out – like he’s locked himself in a vault, and there’s nothing you can do to reach him.
Simple: use simple, concise phrases. “You want to feel connected to him. You long for it.”
Slow: use the pace of your speech to create space in room for deeper emotional experience.
Soft: use a quieter tone to provide comfort and connection.
Client words: used to validate and support the client in their story. Repeating key emotional words can heighten the emotions related to their attachment fears, which can help clients engage with their hurt and sadness instead of their anger and defensiveness. “You feel alone, like he’s not there for you in those moments when you need him the most.”
Working with highly escalated clients can be incredibly challenging, but also incredibly rewarding. If we focus on their anger as an expression of their attachment fears rather than an intentional move to injure, we can start to see the deep bonds these couples have toward one another. Be aware that that working with highly escalated couples means being witness to the horrible things they say to each other. You cannot prevent that, but you can make these moments constructive by putting them into the interactional cycle that brings the couple into treatment; that, ultimately is the goal of working with these distressed, difficult couples.
Print a copy here.

Ian Witter is a certified EFT therapist and EFT supervisor-in-training located in Mission Valley. He would be happy to answer any EFT related questions, and is available for case consultations.
www.ianwitter.com
ian@ianwitter.com